Telemetry Certification Glossary: Top 14 Key Terms To Know
There are a few words you’ll need to know when you take your Telemetry Certification exam. While most of key glossary terms are clinical, and often answered by physicians or nurses in the telemetry unit, it will be wise to study the telemetry terms in advance to get ahead of the learning curve.
The terms you take note on are important, but that’s not all there is to studying for your exam. It’s the desire and experience of a technician that goes well beyond a mere certification glossary. It’s a terrific idea to study the terms, jot down concepts you are struggling with, then do your own research—on the job and beyond.
You’ll learn a lot both at your place of employment and by asking intelligent questions to fellow co-workers, as well as physicians and nurses you’ll be working with.
The telemetry exam cannot take the place of solid on-the-job training, however, you’ll be one step forward in your career if you learn these 14 key terms:
1. Aberrant Ventricular Conduction
Thought to be a phenomenon, Aberrant Ventricular Conduction is defined as intermittent abnormal intraventricular conduction of a supraventricular impulse because of unequal refractoriness of critical prematurity of a supraventricular impulse and bundle branches. (see diagram of Three Fates of PACs).
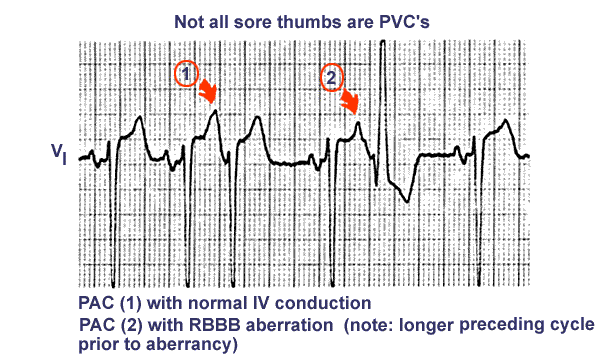
Medical Graph: University of Utah
2. Acute Myocardial Infarction
Acute myocardial infarction is a heart attack. “Acute” is a measure of time. In reference to a disease, it means an abrupt onset.. Acute illness is of short duration and rapid progression and urgent care is often necessary. The time scale depends on the unique disease. An acute myocardial infarction may last a week, while an acute sore throat may last a day.
In contrast, “subacute” indicates longer duration or less rapid change of illness or condition and “chronic” indicates indefinite duration or no change.
3. Atherosclerosis
Progressive thickening and hardening of the walls of arteries as a result of fat deposits on their inner lining. Risk factors for atherosclerosis include high blood pressure (hypertension), high levels of “bad” cholesterol (LDL), smoking, diabetes, or a genetic family history of disease. Atherosclerosis can cause coronary artery disease (angina and heart attacks), as well as strokes.
4. Atrial Fibrillation
An irregular heart rhythm throughout the upper chambers (atria) of the heart. Chaotic electrical signals are generated in superior area of heart. Many patients with atrial fibrillation have no symptoms. Those that do have an uncomfortable awareness of the rapid and abnormal heartbeat (palpitations).
Atrial fibrillation can cause a formation of blood clots (auricular fibrillation) that travel from heart to the brain, resulting in stroke. Atrial fibrillation treatment involves risk-factor control and/or use of medications to slow heart rate to normal rhythm.
5. Atrioventricular (AV) Node (knot tissue)
This AV node, our electrical relay station, controls heart rate and provides electrical signals between the upper and lower chambers of the heart. These signals from the atria must pass through AV node to reach ventricles. The AV node is one of the major elements in the cardiac conduction system
The AV node slows electrical current sent by sinoatrial (SA) node before signal is permitted to pass down through to ventricles along fibers embedded in walls of lower portion of heart. This delay allows atria to contract before ventricles are stimulated.
AV node has a delay which allows for atrial contraction and more filling of heart ventricles (RATE: 40-60 BPM)
6. Bradycardia
A slow heart rate defined as less than 60 beats per minute.
7. Artial Ectopic
An atrial ectopic beat is an extra heartbeat. It means trouble in electrical system of the heart and is caused by a signal to upper heart chambers (the atria) from an abnormal electrical focus.
An ectopic rhythm in pregnancy is an irregular heart rhythm (a pause) because of a premature heartbeat. Also known as premature atrial contraction, extrasystole, or premature ventricular contraction.
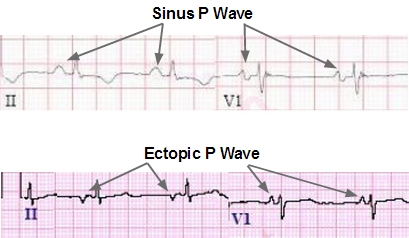
Medical Graph: Healthline
8. Electrocardiogram (ECG and EKG)
The electrical activity recording of heart.
An ECG is a non-invasive procedure. Electrodes are placed on skin of the chest and connected in a specific order to a machine that measures electrical heart activity. Output displays a graph of activity on a computer screen.
T-Wave is ventricular repolarization, meaning it’s the resting phase of the cardiac cycle and there’s no associated activity of ventricular muscle.
Diagnosis of heart attack is made by observation of clinical symptoms and characteristic ECG changes. An ECG can detect areas of heart muscle that are deprived of oxygen or dead tissue (infarction). Before a patient takes medicine that could adversely affect heart function, a baseline ECG is ordered. Follow-up testing occurs at regular intervals to look for any changes.
9. QRS Complex
The QRS Complex is the combination of three (3) of graphical deflections seen on a typical electrocardiogram (EKG or ECG) and is the most central and obvious part of heart tracing. The QRS Complex corresponds to depolarization of right and left heart ventricles; thus representing specific electrocardiogram (EKG) heart ventricular activity. An EKG is done to check for abnormal heart rhythms. Other ‘Complex’ tests include electrophysiologic testing for abnormalities of heart’s electrical system and rhythm monitoring tests (heart event recorders).
10. Sinoatrial (SA) node (Also called sinus node)
The SA node consists of a cluster of cells situated in upper part of right atrium wall of heart where electrical impulses are generated. A major element in cardiac conduction system, the SA node—our heart’s natural pacemaker—controls heart rate and conducts electrical impulses throughout heart muscle, stimulating heart to contract and pump blood.
The electrical signal generated by SA node moves from cell to cell down through heart until it reaches atrioventricular node (AV node), a cluster of cells situated in the center of the heart between the atria and ventricles that serve as a gate to slow electrical current passing into heart.
SA node is the fastest rate of automaticity and is considered a “primary” pacemaker of the heart. (RPM: 60 to 100 BPM)
The portion of autonomic nervous system that controls blood pressure, controls SA node to trigger start of cardiac cycle. The autonomic nervous system can transmit a message to SA node so it can increase heart rate to twice normal pace within only 3 to 5 seconds. This quick response is important during exercise when heart needs to increase its beats per minute (BPM) speed to keep up with body’s intensified demand for oxygen.
When SA node fires, it sends electrical impulse outward to stimulate both atria, manifesting as a P-Wave (Approximately 0.10 seconds in length.)
11. Syncope (pronounced sin-ko-pea)
Partial or complete loss of consciousness with interruption of awareness of one’s surroundings due to a temporary reduction in blood flow and a shortage of oxygen to the brain. When loss of consciousness (lightheadedness or “blackout” episode) is temporary and there’s spontaneous recovery, it’s considered syncope in non-medical terms—fainting. One in every 30 visits to an emergency room is due to syncope.
Temporary impairment of blood supply to brain can be caused by non-cardiac and cardiac conditions:
For our purposes, let’s discuss cardiac causes. Heart conditions that can cause syncope:
- Abnormalities of heart valves (pulmonic valve stenosis or aortic stenosis)
- Irregular heart rhythms (too fast or too slow heart beats)
- High blood pressure in arteries supplying lungs (pulmonary artery hypertension)
- Tears in aorta (aortic dissection)
- Heart muscle disease (cardiomyopathy)
No treatment is necessary for non-cardiac causes of syncope such as postural hypotension, vasovagal reaction, and situational (body reacts to triggers) syncope. Patient often regains consciousness by sitting or lying down and is advised to avoid trigger situations. They’re directed not to strain when eliminating body, to sit when coughing, and to lie down for blood drawing.
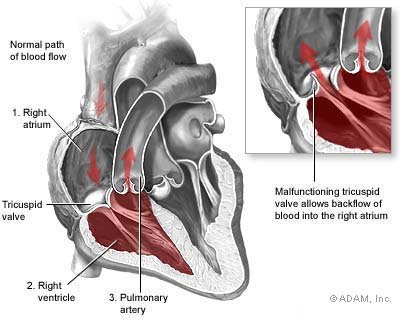
12. Tricuspid Regurgitation
Medical Illustration: New York Times
Tricuspid regurgitation is a heart disorder where the tricuspid valve doesn’t close properly, resulting in blood leak (backward flow) into right atrium (upper heart chamber) when the right ventricle (lower heart chamber) contracts.

Illustration: American Heart Association
13. Ventricular Tachycardia
“Tachycardia” is rapid heart rate defined as greater than 100 beats per minute and ‘ventricular tachycardia’ is a rapid, abnormal heart rhythm that originates from an area of lower heart chamber (ventricle). Ventricular Tachycardia are life-threatening arrhythmias and are associated with heart muscle damage due to coronary artery disease.
14. Wenckebach Phenomenon
Wenckebach phenomenon is a heart block in which a pulse from the atrium periodically does not reach the ventricle. The phenomenon is characterized by progressive prolongation of the “P-R interval” until a pulse is skipped.
Second degree heart block occurs in two (2) varieties: Type I (Wenckebach) and Type II (Mobitz). Wenckebach (Type I) block there’s a decremental conduction; a velocity that slows down until failure of conduction occurs. Mobitz (Type II) an entire block due to reversible conduction block at the level of the AV node.
Telemetry Glossary Terms Are Important To Know, But Your Success Is Up To You
These terms are just a handful of glossary words to start you thinking about your career path. There are much more to learn and study ahead—both by book and on the job training. You’ll find a telemetry position both delightful and challenging.
Many Telemetry Technicians who take a personal interest and desire advancement will be most successful. Your future in cardiac telemetry is completely what you make of it. While learning the glossary terms is critical, it’s just as important to have empathy, emotional strength, and compassion for your patients. There are clinical words to discover, but there’s something to be said about innate character qualities and skillsets in order to provide the best care for your patient.
“Life as a Telemetry Technician is an exciting one. I enjoy participating in continued education—online AND on the job training—it’s both delightful and challenging at the same time. Everything I learn keeps my days interesting.” —Valentyna Patsula, Telemetry Technician, Hospital
Find A Telemetry Technician Certification That Works For You
Most online certifications to become a Telemetry Technician are cost effective and obtainable, accommodating your busy schedule. The exam itself typically lasts 180 minutes and consist of 303 questions. A score of 85% or higher is required to pass. When you pass the exam, you’ll receive a mailed certificate.
The certification process was important and very good process. Most of the questions were clinical which a Nurse or Doctor can answer. It was over the experience of a technician, however, the exam allowed for advanced learning. —Amin Danish, Telemetry Technician, Hospital
Also, your registration number will be listed on our website for employer review. You’re allowed a maximum of three (3) paid exam attempts within six (6) months, after which you must wait a minimum of six (6) months after your third re-test attempt. Once you open exam, you can’t save and quit. Be sure you have a predictable Internet connection and minimal distractions before you begin.
If you’d like to register for an Telemetry Technician exam, download your study guide today and get a jump start at learning the key terms in the telemetry dictionary!